
It goes without saying that nurses are busy. Caring for patients and keeping up with documentation (amidst their many other clinical responsibilities) takes up the majority of their time and resources. However, there are tools that nurses should add to their arsenal, that won’t take more time out of their day, but rather, give time back to them.
An integrated EHR can help nurses in a variety of ways. You can start putting it into practice from day one with these tools:
Surveillance/Evidence Based Content
Find an EHR with a surveillance tool that applies evidence-based practice around clinical decision support. Evidence-based algorithms search the clinical and demographic data in the EHR, take that live, actionable, real-time information, and return it to nurses in a meaningful way to improve outcomes and in turn, the patient experience. Patients who meet certain criteria automatically populate tracking boards that indicate when quality measures are due; show signs of a potential hospital-acquired condition; and provide notifications of out-of-range values, as well as critical medication and transfusion information. A tool like this can be a real time-saver for inpatient nurses, giving them meaningful, actionable data, and helping them to know which patients need their immediate attention.
Comprehensive standard content is available with surveillance boards which already have outcome-based components and rules/algorithms incorporated to analyze data, easing your burden of having to create the content in the first place. A great surveillance solution will have a library of standard surveillance boards, which include the embedded rules needed to comply with clinical quality measures and protocols.
In addition, you will want to find content that provides active and predictive surveillance for early detection of sepsis, VTE, CAUTI, stroke, pneumonia, and other potentially life threatening conditions or diseases. The surveillance board should also monitor patient populations that may be vulnerable, such as patients with a high risk of readmission, patients with specific therapy consults, or patients with restraint orders. This can help improve clinical outcomes, and reduce length of stay.
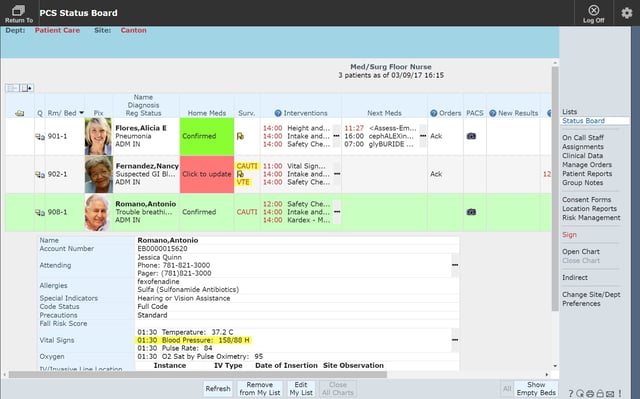
Watchlist
A watchlist can automatically generate a list of patients that need your immediate attention from a quality and patient safety perspective. Watchlists can be built around fall risks, restraints, sepsis, or any other potential danger you deem important. This tool can save nurses a tremendous amount of time over manually reviewing information and creating lists. With manual lists, as soon as they are printed off, the information is outdated. An electronic watchlist created in real time gives nurses the most recent patient information at their fingertips, and also lends itself to patient safety by having up-to-date lists of patients that nurses can monitor quickly and more completely.
.jpg?width=640&name=surveillanceglobalwatchlist_QM%20(1).jpg)
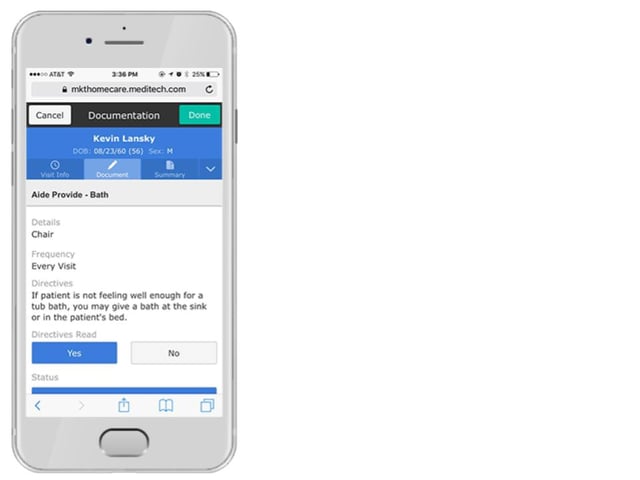
Mobile Documentation
Find an EHR that has a mobile component which will enable nurses to conveniently review and document care from smartphones using modern web browsers, saving them time from having to walk back and forth between the nurses station and the patient's room. The great thing is that they most likely already use a smartphone, so they’re very familiar with its functionality. Whether a nurse, LPN, aide, or other care provider, your clinicians can use their smartphones for performing tasks such as quick medication verification and care intervention documentation.
Critical Care Flow Sheets
Find a solution that has a critical care flow sheet integrated into the EHR. It will help nurses in these settings to better understand the patient's journey and deliver appropriate care quickly. For example, whether their patient arrived through the ED or is currently on a ventilator in the ICU, providers will have clear, accessible information on the patient’s care progress all in one place, saving them time on documenting care. Nurses can also ‘live’ in the flow sheet, and review labs, meds, and notes, all while collecting information from monitors, ventilators, EKG readings, and administering and titrating medications.
Case Management
A solution with case management functionality helps nurses to facilitate smoother transitions of care and reduce readmissions risks by tracking data from monitoring devices, such as bluetooth-enabled scales and blood pressure cuffs, so they can quickly identify those at risk of readmission and those with changes in condition. This gives them a chance to reach out and intervene before a costly visit to the ED or an unnecessary inpatient stay.
Integrated Home Care
An EHR with an integrated home care solution enables nurses to share allergies, medications, problems, and other information across the spectrum. Home care agencies and hospitals can then work together as a team to improve care transitions, treat chronic conditions, and avoid readmissions.
This type of integration benefits both the patient and their care team. With all of the patient’s information in one place, clinicians can view any request for orders and approve them, as well as approve any care plans. Home care nurses also save precious time by not having to go to the fax or snail mail route. Agencies can also use their own smartphones to view their schedules, aid documentation, and view a patient's diagnosis, procedures, medications, or other important patient information.
Nurses are at the forefront of care and need strategies to make their lives easier, save time, and of course, uphold the best patient care possible. Using these tools will help them do just that, and help keep the patient at the center of it all.
Interested in how nurses and nurse leaders can improve safety, even in the midst of the opioid epidemic? Read our special report.




