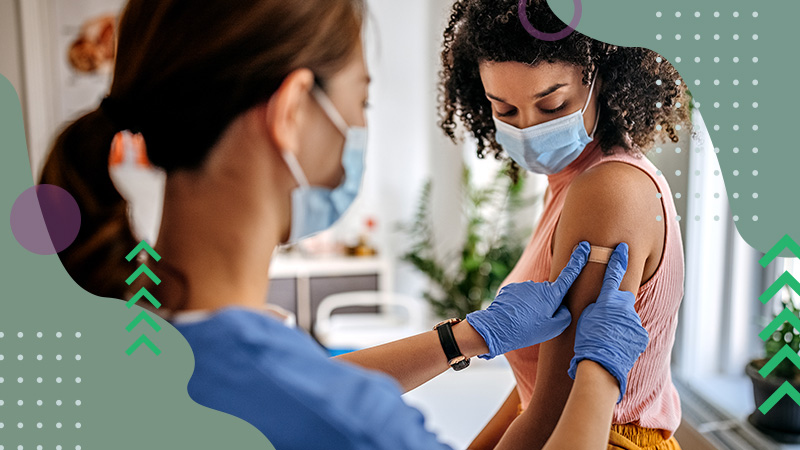
At the peak of the coronavirus surge in Massachusetts, I took a leave of absence from my position as a Marketing Solutions Specialist to care for COVID-19 patients. I’m a young nurse with an active license and felt I had a responsibility to help my community. Volunteering at Boston Hope Medical Center (BHMC), the field hospital constructed in the Convention and Exhibition Center, gave me the opportunity to make a difference as this poorly understood pandemic raged on. Little did I know, the experience would provide unique insight into the power of a well-designed EHR in managing the turmoil surrounding clinical care during a public health crisis.
At the peak of the coronavirus surge in Massachusetts, I took a leave of absence from my position as a Marketing Solutions Specialist to care for COVID-19 patients. I’m a young nurse with an active license and felt I had a responsibility to help my community. Volunteering at Boston Hope Medical Center (BHMC), the field hospital constructed in the Convention and Exhibition Center, gave me the opportunity to make a difference as this poorly understood pandemic raged on. Little did I know, the experience would provide unique insight into the power of a well-designed EHR in managing the turmoil surrounding clinical care during a public health crisis.
Caring for COVID-19 patients at Boston Hope was unlike any clinical experience I had ever had. Looking back, I realize the challenges revealed by this almost-apocalyptic environment had notable similarities to issues clinicians have faced for decades.
Timing is everything
Every task took longer than expected due to increased infection precautions and the mayhem of patient care. (I had nine patients at one point.) Thus, it was especially important that the EHR didn’t place additional time constraints on already overburdened clinicians. I learned that these EHR features are invaluable during a crisis:
- Any documentation shortcut, quick text field, or formatted data table is a breath of fresh air.
- Point-of-care and other mobile tools save a huge amount of nursing time, because entire workstations don’t have to be sanitized between patient rooms.
- An easy-to-use, intuitive, and streamlined EHR allows nurses coming from outpatient settings and non-clinical roles to quickly learn the software.
- Having the information I need where I need it allows me to focus on attending to patients, not the EHR.
As I said to my MEDITECH colleagues when I returned from BHMC: “When everything is chaotic, the EHR is one thing that shouldn’t be.”
Getting the word out
The age-old problem of care team communication became a physical reality at the field hospital. Treating COVID-19 patients exclusively meant wearing full PPE for the entire shift. While I am grateful to have had sufficient PPE, relaying information quickly and accurately is challenging when words and body language are muffled by gowns, gloves, N95s, and face shields; instead, we relied on digital tools. Comment fields, care team bulletin boards, acknowledgment indicators, and direct provider messaging can provide the communication pathways we need to keep patient care as coordinated and timely as possible.
Another communication challenge facing clinicians and healthcare leaders was informing the entire staff of rapidly changing protocols. In treating a condition no one has seen before, with a flood of recommendations from researchers and the CDC, protocols were being updated almost hourly. For example, one particular medication protocol changed three times over the course of the day shift. The ability to reference those protocols within the system and disseminate them through clinical decision support keeps everyone on the same page — even when the pages are turning quickly.
Addressing healthcare inequities
In working with patients at Boston Hope, I observed a well-known but often hard-to-see fact: Health inequity in our communities is a critical problem that demands immediate attention. Coronavirus disproportionately affects minority and high-risk populations. Among the patients I cared for at Boston Hope, about 80 percent didn’t speak English well enough to receive care without a translator. Many lived in crowded home environments, others faced homelessness long before the pandemic, and some had lost their housing due to their positive COVID-19 status.
Barriers related to inadequate housing and other social determinants of health have existed long before COVID-19. This pandemic is a call to action for healthcare leaders to help address these damaging factors through technology. For example, surveillance tools can be used to flag at-risk individuals proactively, and registries can identify care gaps. Our patients and communities are looking to healthcare organizations for help like never before; we need to leverage the best digital tools available to meet those demands.
Supporting clinicians on the front lines
Serving on the front lines of the COVID-19 pandemic, I saw loss, fear, trauma, and chaos.
But I also saw resilience, compassion, camaraderie, strength, and mutual respect among patients and providers alike.
The experience has transformed my perspective on the work we do here at MEDITECH. Our EHR plays a crucial role during healthcare crises; all of the features I mentioned are available in Expanse and are making a real, human impact on patients and clinicians alike. I hope to use these lessons learned to better support my fellow nurses, the rest of the care team, and anyone who has the privilege of making a patient’s day just a little bit brighter.
Sign up for the webinar below to hear more of Leah's story, as she sits down with MEDITECH AVP Cathy Turner, RN-BC, to discuss the difficulties clinicians face while caring for patients during a public health crisis, and how the right EHR can help to alleviate these challenges.